Osteoarthritis of the ankle, caused by wear and tear of the joint, results in swelling, pain, and foot deformity. Recommended treatment options include total joint replacement and arthrodesis. At the Paley Institute, we offer an alternative: joint preservation techniques that retain the patient’s natural ankle joint and ankle motion.
We use a technique that involves distraction of the joint with external fixation. This procedure is a viable alternative to arthrodesis and / or joint replacement, with the added benefit of restoring normal joint anatomy. The technique uses the principle of ligamentotaxis to restore normal joint space, improving joint loading, and providing an environment in which the joint cartilage can recover.
Indications for ankle joint distraction include:
- Congruent joint surface
- Ankle pain
- Reduced ankle mobility
- Moderate to severe osteoarthritis
Joint distraction may also be efficacious in treating avascular necrosis of the talus.
Ankle distraction works by transferring the weight-bearing forces from the cartilage to the external fixator. This relieves pressure on the cartilage, allowing it heal. Weight bearing in the fixator also allows for continued intra-articular fluid pressure and increased synovial fluid, providing further cartilage restoration. Fixation also allows for reduction in the subchondral bone density, increasing the resiliency of the joint. These changes allow the osteoarthritic cartilage to regenerate.
Our Method
Drs. Paley and Lamm developed multiple improvements upon the initially published techniques for ankle distraction. First, they built an ankle distractor with a hinge that allows patients to perform range-of-motion exercises throughout the distraction treatment. Second, they included additional surgical procedures to increase range of motion, eliminate impingement, improve stability, and improve joint orientation. The modifications are as follows:
- Hinged ankle joint distraction
- Allows joint range-of-motion exercises during treatment
- Correction of osseous alignment during osteotomy
- Soft tissue releases
- Corrects soft tissue contractures
- Resection of osteophytes and osteochondroplasty
- Treats joint impingement
Surgical Procedure
Blocking Osteophyte Resection
If dorsiflexion (pulling the foot upward) is limited by osteophytes (bony outgrowths that develop when cartilage deteriorates), we will resect the osteophytes through an anterior (front of the foot) incision. If plantar flexion (pushing the foot downward) is limited by osteophytes, they are removed via a posterolateral (to the side and to the back) incision. To prevent osteophytic recurrence, bone wax is applied to the bone. Nonsteroidal anti-inflammatory drugs (NSAIDs) are administered postoperatively for 6 weeks to inhibit bone formation. However, NSAIDs are not administered if an osteotomy is performed during surgery.
Equinus Contracture Release
Equinus contracture is released by performing a gastrocnemius recession, a gastrocnemius-soleus recession, or an Achilles tendon lengthening. We prefer gastrocnemius recession or gastrocnemius-soleus recession, in order to maintain muscle strength. A posterior capsule release may be necessary to restore ankle joint range of motion. A tarsal tunnel decompression is often necessary to prevent nerve entrapment. When acute release does not reduce the equinus, it can be corrected gradually via distraction.
Ankle Joint Realignment
Ankle joint malalignment due to deformities such as valgus and recurvatum may be the underlying cause of the ankle joint degeneration. To preserve the ankle joint, we will perform reorientation procedures, including osteotomy (surgical bone cut). Correction is usually done using a supramalleolar osteotomy. If there is incongruence between the tibia and fibula, then the tibia can be lengthened or the fibula shortened to restore normal ankle anatomy. We will address any subtalar joint contractures at the time of realignment and distraction. This can be done acutely via release or gradually via the external fixator.
Application of Hinged External Fixator
The hinged external fixator is applied to the foot and tibia. We prefer to simultaneously distract both the subtalar and ankle joints acutely. This is done by applying distraction between the tibial and foot fixation before inserting wires into the talus.
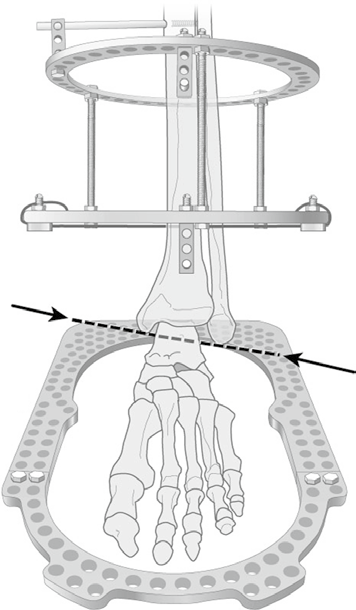
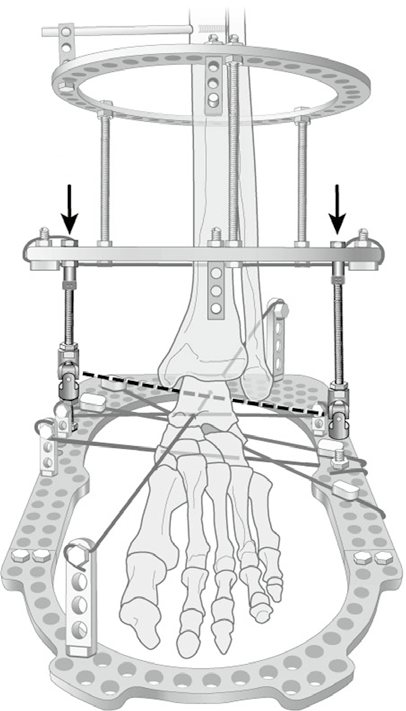
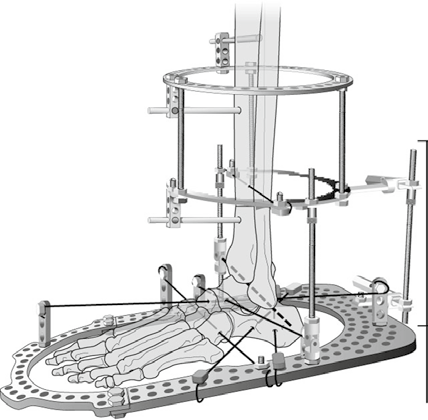
The patient starts distraction at a rate of 1 mm per day on postoperative day 1 for a total of 5 days. The goal is to achieve 8-10 mm of distraction. The external fixator is then maintained for 3 months while allowing weight bearing as tolerated. The patient performs daily ankle range of motion exercises and should attend physical therapy three times a week.
Summary
In a published study, Dr. Paley and Dr. Lamm reported their results on 32 patients who underwent ankle joint distraction and found 78% had maintained their ankle range of motion and had none to occasional pain that could be managed with NSAIDs. Only one patient required an ankle fusion and only one was converted to an ankle joint replacement. These results suggest that Dr. Paley's and Dr. Lamm's approach improves upon the results of this procedure.
Ankle joint distraction is a strong viable alternative to ankle arthrodesis or ankle replacement. A congruent, painful, mobile, and arthritic ankle joint treated with this technique can achieve good results. The à la carte approach developed by Drs. Paley and Lamm results in more successful outcomes using this approach.
For more information, see Joint Distraction for Special Conditions