
News & Events Click through below for a glimpse at our latest news & events.
What is Paley care?
Our mission is to provide the best care to patients with bone and joint conditions, from minor fractures to the most complicated limb or spine deformities. As the world leaders in reconstructive orthopedic surgery, we provide patients with the most advanced, innovative treatments customized to their individual needs. We are committed to raising the standard and outcome of orthopedic surgery worldwide.
For over 30 years, we have been providing exceptional healthcare to patients from all over the nation and around the world. Let us provide you with the care that you deserve.
No other medical destination in the world can compare to the Paley Orthopedic & Spine Institute. Physicians, specialists and insurance companies around the world refer their patients to the Paley Orthopedic & Spine Institute particularly when the diagnosis is unclear, the procedure is insurmountable, or even the most common conditions warrant the best of care.
The world-class surgeons and the personalized approach of the Patient Care Coordination Team provide comprehensive second opinions and consultative support for referrers to assure patients achieve the right diagnosis and the right access to care the first time around. As a Center of Excellence in highly complex orthopedic clinical services, the Institute seeks global partnerships to expand its footprint and advocacy through referral treatment, professional consultancy, and physician training that supports the entire lifespan of families in need of orthopedic care.
The level of clinical expertise equals the overflowing compassion and personalized experience delivered by the Patient Care Coordination Team. Families can trust they will receive the world-class comprehensive medical care, and world-class compassion.

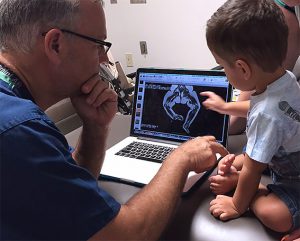


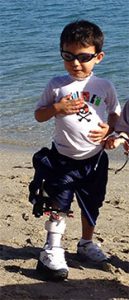









World Class Care Paley Orthopedic & Spine Institute patients come from all over the world.
Click on the purple dots on the map below to read patient stories.
Map Display Type
You can choose what patient data to display on the map above by using the drop-down box below.
-
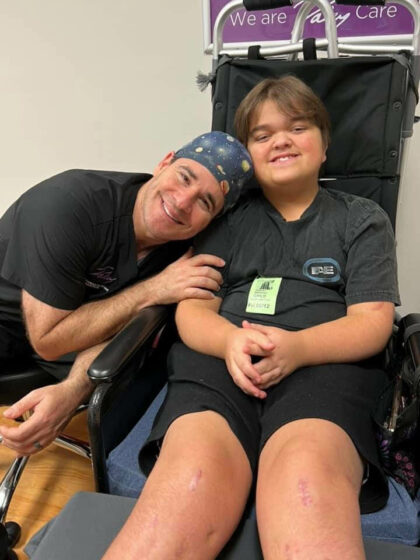
Kory New Jersey, USA Achondroplasia
"My son has achondroplasia and has completed all 4 phases of limb lengthening as of May 14, 2023: three bilateral 4-segment leg lengthenings and one bilateral arm lengthening for achondroplasia. He began his journey in 2015, being the first pediatric patient to have a custom-made precise rod implanted in his femurs at age 6, June…
Learn more about Kory's case -

Andrew Florida, USA Limb Lengthening & Deformity Correction
Dr. Paley, I wanted to say thank you for all you have done for me over the years, starting in Baltimore, and now in Florida. I love my new life and I’m SO incredibly happy with the results. I honestly believe I am alive today because of you. You helped me get through some very…
Learn more about Andrew's case -
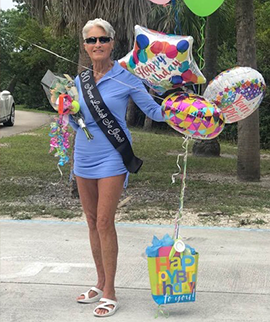
Barbara Florida, USA Treatment Strategies
Dear Dr. Paley, I had originally seen Dr. Minus as I was having problems with my right knee. He ordered an MRI and discovered that I had a torn meniscus. Dr. Minus recommended physical therapy to see if that would correct my problem. Sadly, the blood supply is limited in that area and it did…
Learn more about Barbara's case -

Doug Florida, USA Cervical Stenosis
I’ve been a patient of Dr G’s for about 4 years. From my initial visit it was clear that his goal was to get me as comfortable as he could. He asked more questions than most… seemed to care more… and then he came up with a plan. For about 2 years he kept me…
Learn more about Doug's case -

Mary Florida, USA Femur Fracture
My name is Mary. Just a little background on where I was before my injury – Most of my life I was an avid athlete, runner and tennis player. Ten years ago I gave up running to save my knees, and fell in love with speed walking. Eighteen months ago I was trying out a new pair of…
Learn more about Mary's case -

Everly Salina, Kansas, USA Congenital Femoral Deficiency
Everly was born with Fibular Hemimelia and Congenital Femoral Deficiency in her left leg — she had lacked ankle structure, had a dislocated hip (not born with it), and did not have a fibula. After seeing multiple specialists in the United States we finally met with Dr. Paley and his team when Everly was 6-months…
Learn more about Everly's case -

Kevin Turin, Italy Tibial Hemimelia
Kevin was born on December 5, 2017 in Turin italy with a malformation in his right leg. The whole thing had not been diagnosed during pregnancy and was only discovered at birth. The pathology is called TIBIAL HEMIMELIA, Kevin was born without the patella and without the tibia and his leg is 4cm shorter and…
Learn more about Kevin's case -

Mitchell New Mexico, USA Tibial Hemimelia
I wanted to write you and thank you for the care you and your team gave our son, Mitchell. He had some “minor surgeries” over the years, but in 2011 you performed a femoral and tibial lengthening surgery on him. During that summer we moved to Jupiter so we could have all the physical therapy…
Learn more about Mitchell's case -
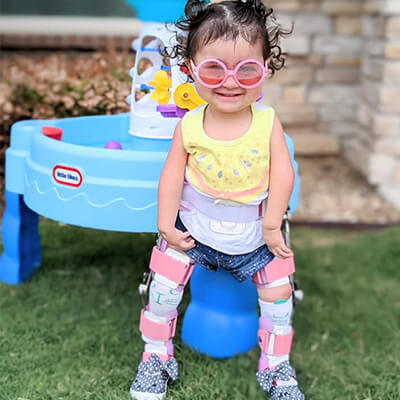
Lucy Lubbock, Texas, USA Arthrogryposis
When Lucy was born she couldn’t move anything but her head. After being told by doctors in our area that they couldn’t start treatment on her legs until she was 18 months to 2 years old, we were determined to find another opinion. Thankfully we found Dr. Feldman and his therapy team. Lucy arrived at…
Learn more about Lucy's case -

Griffin Arkansas, USA Clubfoot
At our 20 week ultrasound, it was suspected that our son, Griffin, would be born with bilateral clubfeet. We spent a good portion of our pregnancy researching Clubfoot. When Griffin was born, we were told by multiple pediatricians at the hospital his feet were ‘normal’. As you could imagine, this was a relief, but with…
Learn more about Griffin's case -
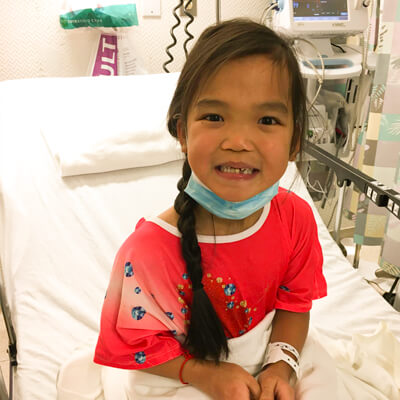
Hannah Mogadore, Ohio, USA Larsen Syndrome
Our story began in July 2019 when we brought home the most beautiful, spunky, smart daughter who would just be turning eight years old! She was born with a rare “superpower” called Larsen Syndrome. She had undergone eight other surgeries in her country, without parents navigating things. Some of them, I am sure, were helpful…
Learn more about Hannah's case -

Alexa Florida, USA Scoliosis
When my family found out that my daughter had scoliosis and would need surgery, we knew we were at a crossroads. We were concerned about finding the right doctor, about how Alexa‘s life would change following the surgery, and about even the risks of the surgery itself. We interviewed several doctors in the south Florida…
Learn more about Alexa's case -

Jamie Cayman Islands Brachymetatarsia
After years of discomfort and pain for a birth defect, I was completely unaware of. I am eternally grateful for Dr. Lamm and the Paley Orthopedic Institute. Over the last three years, I had seen numerous specialists both within and outside of the USA and no one could give me answers to relieve my…
Learn more about Jamie's case -

Meagan Alexandria, VA, USA Joint Preservation & Replacement
I was referred to Dr. Minas in May 2019 after an unsuccessful autograft revealed that my 33-year-old knees had more damage to the bone than the procedure could fix. It was recommended that I get an allograft procedure, which was a specialty of Dr. Minas’ and his office quickly reached out to set up a…
Learn more about Meagan's case -

Davely Texas, USA Tibial Hemimelia
Davely was born with bilateral Tibia Hemimelia in 2015, due to the abnormal orthopedic development in her legs, she had to have her right leg below the knee amputated at 18 months. In order to save her Left leg from being amputated as well in Texas, we came to Florida, to The Paley Institute in…
Learn more about Davely's case -

Olive Fort Mill, SC, USA Limb Length Discrepancies
Olives story is very similar to many here. After visiting doctors in the NY/NJ/Delaware area we were about to amputate our daughters leg and foot. My mother in law had heard of Dr. Paley I believe from Oprah or an article and gave us his information. I emailed Dr. Paley telling him we are about…
Learn more about Olive's case -

Alexa Tibial Hemimelia
Alexa was born with Bilateral Tibial Hemimelia. We sought out treatment in Chicago, Dallas, as well as at The Paley Institute. Dr. Paley was the only one of the three that recommended reconstruction versus bilateral amputation. Alexa presents two different types of Tibial Hemimelia. She has Paley type 1A in her left leg, and Paley…
Learn more about Alexa's case -

Mike New Hampshire, USA Joint Preservation & Replacement
Dr. Minas was recommended to me by my primary care physician about 10 years ago after I injured my knee playing rugby. Being a rugby player, I dismissed it, took a few aspirins, and played for another 6 years before the pain became too great to continue. I finally broke down and decided to look…
Learn more about Mike's case -

Jayde Florida, USA Hip Dysplasia
When Jayde was a small child, I noticed that her feet turned slightly inwards as she walked and while standing. I took her to her pediatrician, who in turn, referred her to an orthopedic specialist. Jayde was diagnosed with Tibial Torsion. The doctor told me that the condition was benign and that “it would correct…
Learn more about Jayde's case -

Jesse Sarasota, FL, USA Joint Preservation & Replacement
Twenty years ago, at the age of 46, I was told that I needed a total knee replacement. At the time, I was managing my busy orthodontic practice, coaching Little League baseball, and raising a young family. The news was devastating. As I traveled the country seeking other opinions, I became accustomed to hearing the…
Learn more about Jesse's case -

Liana Pittsburgh, PA, USA Joint Preservation & Replacement
When an athlete comes to the end of his/her career, there is an emotional and physical transition process that takes place. With a career-ending injury, however, the cause of this change is sudden. An abrupt and unexpected halt leaves no time or opportunity to plan for a transition out of the sport. An athlete is…
Learn more about Liana's case -

Maddie Gastonia, NC, USA Perthes Disease
Our journey with The Paley Institute began almost 10 years ago when we sought a second opinion with Dr. Paley regarding the management of Maddie’s Perthes disease at 4 1/2 years old. Maddie was a young 19 months when her left femur head lost blood supply. We never imagined her disease process would be so complex. …
Learn more about Maddie's case -
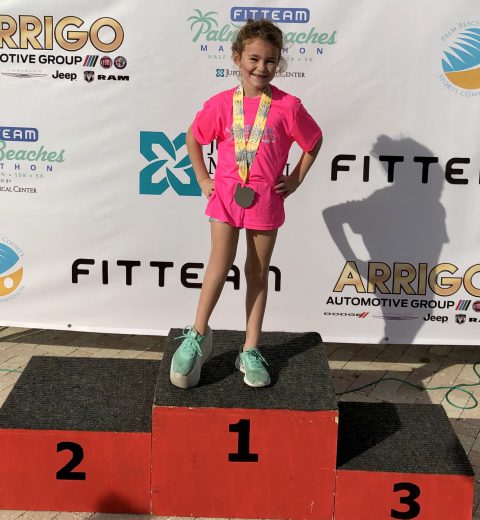
Sadie Congenital Femoral Deficiency
At 3 days old, Sadie was diagnosed with Congenital Femoral Deficiency. We were not given any options at that time to correct anything with her leg or hip and had never heard of this condition until that day. We found Dr. Paley online a few months later and first met with him when Sadie was…
Learn more about Sadie's case -

Jean West Palm Beach, FL, USA Joint Preservation & Replacement
I am 64 years of age, and broke my left ankle in three places, 35 years ago while roller skating. The plates and screws were removed years later, but I developed post-traumatic arthritis over the course of years with severe cartilage loss with bone on bone in the tibiotalar joint. I was a candidate for total ankle…
Learn more about Jean's case -

Graham Covington, GA, USA Ollier’s Disease
At the age of 2, Graham was diagnosed with Ollier’s Disease. Only 1 out of 100,000 are diagnosed with this rare disease. Currently, it is affecting Graham’s growth plate where his femur and knee meet causing him to have a short left leg. At the age of 5, he had surgery in Atlanta, Georgia to rotate…
Learn more about Graham's case -

Mara Madrid, Spain Congenital Pseudarthrosis of the Tibia
Mara was born as a very healthy baby, and it was a big surprise when during her 5-month revision, the pediatrician told us she had noticed a weird bend of her right leg and that a traumatologist should check it up. A week later and after x-rays were taken a sort of nightmare started for us,…
Learn more about Mara's case -
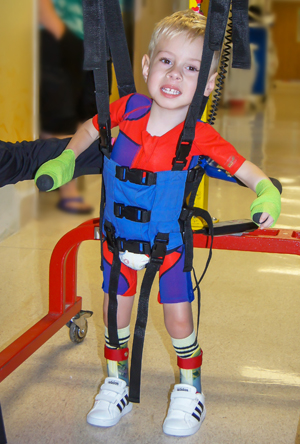
Ryland Arthrogryposis
Ryland was born in 2015 in Wyoming. He was life flighted to the NICU in Denver Colorado, it was there that he was diagnosed with Arthrogryposis Multiplex Congenita or AMC and severe scoliosis. AMC is a non-progressive congenital disorder that often has no ideology as to why it occurs. Babies born with AMC are affected in…
Learn more about Ryland's case -

Andrea Scoliosis
Hi, my name is Andrea and I am 16 years old. I am from Miami, Florida and was raised by my two parents who were born in Venezuela. At the age of nine, I was diagnosed with Scoliosis. It started very mild, but the more I kept growing, the more my scoliosis increased. I went…
Learn more about Andrea's case -

Liddy Achondroplasia
When telling most people my story, I tell them to imagine me standing in front of them being around 3'8". That is what life would have been for me if I hadn't encountered Dr. Paley and underwent limb lengthening. Because of Dr. Paley, I confidently walked out of the Paley Institute a tall 4'11", thanks…
Learn more about Liddy's case -
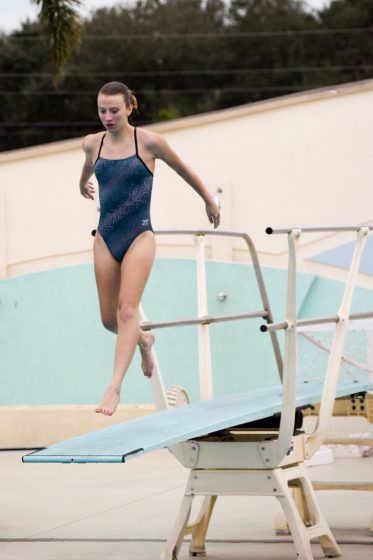
Amy Fargo, North Dakota, United States Perthes Disease
I dove competitively all throughout middle and high school. Dealing with hip pain throughout those years I was still able to finish 3rd in the State my senior year. Diving throughout college now at Nova Southeastern University in Fort Lauderdale, FL with a club team and the college masters division, my hip pain came back…
Learn more about Amy's case -

Olivia Chantilly, Virginia, United States Fibular Hemimelia
When our daughter Olivia was born, my wife Maria and I were shocked to learn that she only had three toes on her right foot and a fairly obvious ankle deformity. Without any prior knowledge of this condition, we were advised by the on-call orthopedic surgeon in the hospital that she believed Olivia had a…
Learn more about Olivia's case -
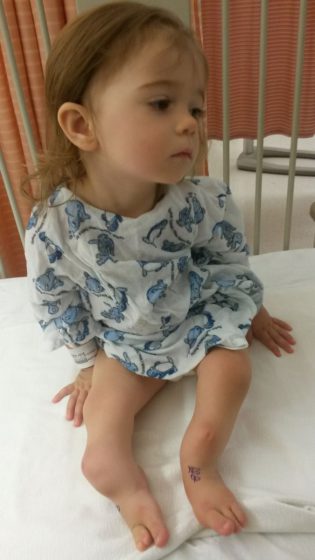
Julia Lublin, Poland Fibular Hemimelia
**Translated from Polish**Julia was born on July 24, 2013 with bilateral fibular hemimelia. Per Dr. Paley, “she had very severe fixed equinovalgus deformities of both legs, the right was worse than the left.” She has three toes on each foot and in addition, the tibia bones were bent and a lot shorter. After birth we…
Learn more about Julia's case -
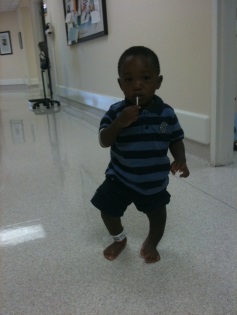
Wekem Accra, Ghana Congenital Pseudarthrosis of the Tibia
Wekem was born in January 2010 with what his local doctor had diagnosed as congenital pseudo-arthrosis. In simple terms his left tibia was short and curved as a false joint. In addition he had a malformed double toe on the same left leg/foot. This was really a shock to us. We spent about 9 months…
Learn more about Wekem's case -
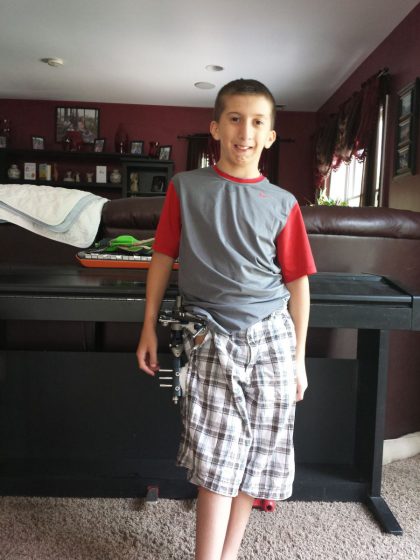
Warren New York, NY, United States Perthes Disease
and after we would go for a ride in the car I would notice he couldn't move very well. He was still playing soccer but he just couldn't move as well as he used to. Warren has a very high tolerance for pain so he never complaint about it, so I really didn't know he…
Learn more about Warren's case -

Vincenzo Bari, Italy Arthrogryposis
Hello, I am Vincenzo and I am 22 years old, I’m an Italian male with a very rare condition that it seemed nobody had ever heard of and there was no cure. The name of my disease is “arthrogryposis”, a disease that in most cases affects the upper and lower limbs, I had both from…
Learn more about Vincenzo's case -

Tristan New York, NY, United States Perthes Disease
When we found out about our son’s diagnosis, we were devastated. Tristan was a big, strong, fast boy who looked indestructible. No way this could be true. And what was worse, Tristan was 10 years old when his injury occurred, and from everything we were able to research about his injury, the older your child…
Learn more about Tristan's case -

Sylvie Austin, Texas, United States Congenital Pseudarthrosis of the Tibia
Sylvie was born on November 2, 2012. At the hospital we noticed that her left lower leg had a pronounced bow, but all of the doctors and nurses told us that this was normal for a newborn and that it would straighten over time. Four months later several café-au-lait spots had appeared on Sylvie’s skin…
Learn more about Sylvie's case -

Stephanie New York, NY, United States Scoliosis
Hi, my name is Stephanie and at a very young age I was diagnosed with scoliosis. My scoliosis progressively got worst the more I was growing. My parents took me to see Dr. Feldman when I was twelve years old in 2011; he told us that surgery would be the best answer. It was an…
Learn more about Stephanie's case -

Sean Ireland Congenital Femoral Deficiency
Our son Sean was born in March 2004. His right femur hadn’t grown. The only options given to us in Ireland, and indeed by many doctors in the E.U, were to amputate his right foot and/or rotate his right leg.No one told us about limb lengthening.We researched ourselves and thank God every day that we…
Learn more about Sean's case -
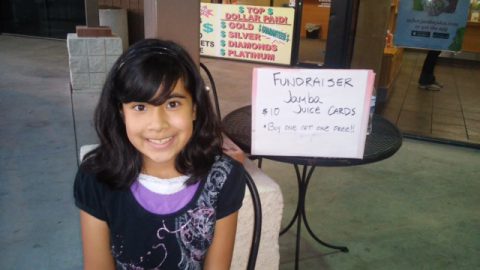
Savanah Phoenix, Arizona, United States Multiple Hereditary Exostoses
My daughter Savanah was about 18 months when she was diagnosed with MHE. Since then she's had 5 surgical procedures. Ranging from removing a bump underneath her fingernail here in Phoenix to major surgery on her hip with Dr. Paley.We were seeing a Orthopedic Surgeon here in Phoenix Children's Hospital and we were continually told…
Learn more about Savanah's case -

Sara New York, NY, United States Multiple Hereditary Exostoses
As I was reading all the reviews before going to the first appointment, I thought that the Paley Institute could do amazing things with children, but as an adult I wouldn't be that lucky. After years of frustration attempting to get help, I didn't honestly expect that anyone would be able to help me. I…
Learn more about Sara's case -

Rosana Venezuela, South America Growth Arrest
My name is Rosana and I follow Dr. Paley all the way from Venezuela. Why you should ask? I was involved in a car accident in 2001. I suffered multiple fractures and I nearly lost my life. Fortunately I was able to overcome the most serious injuries, but I was left with a problem in…
Learn more about Rosana's case -

Robert Patchogue, New York, United States Achondroplasia
As a father of a child with medical issues you only want the best care and the most knowledgeable and compassionate people on your side every step of the way. To say we have received that from the Paley staff is an understatement. We heard that Dr. Paley was the best surgeon for our son's…
Learn more about Robert's case -

Reyli Laredo, Texas, United States Arthrogryposis
On a heavenly October 11, 2005, we were expecting our first-born baby boy with all the joy that new parents experience. His father talking away about how his son would play basketball professionally and I was filled with hope of witnessing all of my baby’s firsts! I spent months readying his room, toys, and getting…
Learn more about Reyli's case -

Paul New York, NY, United States Arthrogryposis
Paul is the cutest, best kid ever. He’s funny. He’s smart. He’s got great dance moves. Every one loves him and he is known as the mayor wherever he goes. He’s a great kid. So all greatness aside, he was also born with a host of medical issues. Upon delivery, the nursing staff noticed that…
Learn more about Paul's case -

Nazanin Urmia, West Azerbaijan Province, Iran Fibular Hemimelia
What I write for you is not consent, it is a letter of introduction to the great men that have great efforts to serve humanity and bring hope to the lives of disabled people.I am Shahram from Iran. My second daughter was born in third of January 2008, with congenital anomalies, Fibular Hemimelia, and the…
Learn more about Nazanin's case -

Nina Oakland, California, United States Post-Traumatic Growth Arrest
Nearly 40 years ago, my left leg was crushed in an auto accident. When I pulled my leg out, I saw nothing attached past my left knee. Instantly, I saw myself as an amputee.Hospitalized for 3 months, I had 6 surgeries for stabilization, skin grafts after debridement, which is removal of bone fragments, soft tissue,…
Learn more about Nina's case -

Nadine New York, NY, United States Hip Dysplasia
After years of right groin pain which was worsening in frequency and severity since my second pregnancy, I was seen by my local orthopedist and diagnosed with a tear of the right labrum. Upon referral to a hip specialist for surgical consultation and subsequent review of hip/pelvic x-rays, a diagnosis of bilateral acetabular dysplasia was…
Learn more about Nadine's case -

Maya Rabat, Malta Fibular Hemimelia
Maya was born in January 2002. She appeared to be a perfectly healthy baby. The middle toe of her left foot, however, struck my attention right from the start. It was thinner and smaller than the other toes. When I pointed this out in hospital I was told that this resulted from being cramped in…
Learn more about Maya's case -

Maja Lublin, Poland Tibial Hemimelia
(translated from Polish)Maja was born March 23, 2014 (40th week of pregnancy) with Tibial Hemimelia. Maja was born with right tibial hemimelia with a completely dislocated patella, total tibial aplasia, duplication of femoral condyle, dislocated foot and ankle in equinovarus, and two-toed foot. The other leg is completely normal. We knew of the birth defect…
Learn more about Maja's case -
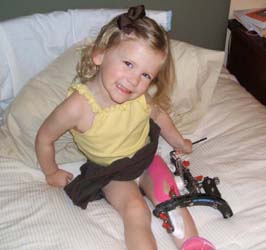
Lillie Augusta, Georgia, United States Congenital Femoral Deficiency
Our little girl was diagnosed with Proximal Femoral Focal Deficiency when she was born. We saw Dr. Paley when she was nine months old and he put our fears to rest!He immediately had a game plan in place and assured us he could help our daughter. She had a hip and knee surgery with him…
Learn more about Lillie's case -

Kristen Charleston, South Carolina, United States Achondroplasia
My parents weren’t familiar with the words Achondroplasia, short stature or dwarfism until I was born. Many people told them that I was not going to ‘thrive.’ Very little was known about my condition at that time, leaving them in the dark about what my future may hold. Saving every article and pamphlet she could…
Learn more about Kristen's case -

Kelly Tempe, Arizona, United States Fibular Hemimelia
Our daughter, Kelly, was born with Fibular Hemimelia. We were told by numerous orthopedic surgeons that we should amputate her right leg at the knee. We were lucky enough to meet with Dr. Dror Paley, and now, 17 years later, we have made the journey through several limb lengthening and deformity correction procedures.The end result…
Learn more about Kelly's case -

Kaitlyn Maryland, United States Multiple Hereditary Exostoses
Our daughter, Kaitlyn, was diagnosed with MHE at 2 years old. We first noticed some bumps on Kaitlyn’s ribs just before her 2nd birthday, October 2015. We had her pediatrician order an X-Ray and a sonogram. The results came back: the bumps were bone, but no one could explain why this was occurring. We weren’t…
Learn more about Kaitlyn's case -
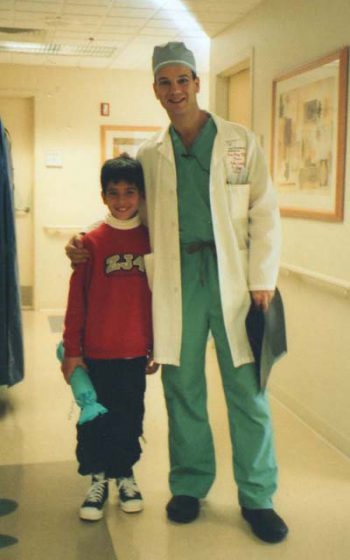
Juan Mexico City, Mexico Tibial Hemimelia
I was born in Mexico City and I am currently a 17 year-old student graduating from high school. I was born with a congenital birth defect. My left leg was slightly shorter than my right leg. My parents sought help immediately after they noticed there was something wrong with me. After doing their research, I…
Learn more about Juan's case -

Josh Ohio, United States Congenital Femoral Deficiency
Dr. Paley,I know it's been many years since I've seen you face-to-face but I do remember that you are the man who helped me to walk. I wanted to personally thank you for making a normal life possible for me.Thank you so much for the knowledge and skill that you invested into my leg to…
Learn more about Josh's case -

John Texas, United States Perthes Disease
In October 2014, John Thomas was diagnosed with Perthes. The doctor’s diagnosis was a wheelchair for around 2-3 years, since we were in the second phase. We sought a second opinion from Dr. Paley. John Thomas had the core decompression procedure in Feb. 2015 by Dr. Paley. He slept in a brace 24/7 except for…
Learn more about John's case -
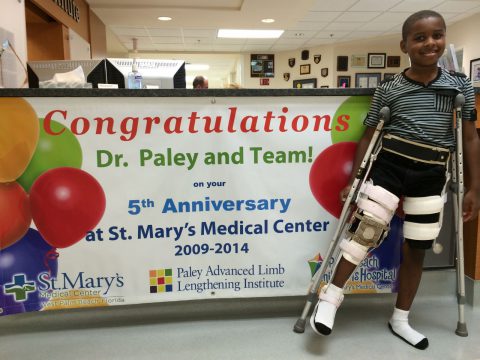
Jabari Columbus, Georgia, United States Congenital Femoral Deficiency
Our three-year old son, Jabari, was born with Congenital Short Right Femur. We were told by a local surgeon that amputation of his right leg and wearing a prosthetic was his only option. Well, his options expanded tremendously when we found Dr. Paley with the click of a computer mouse. Dr. Paley is a genius,…
Learn more about Jabari's case -

Hope Tequesta, Florida, United States Fibular Hemimelia
There is Triumph in AdversityWhile I was busy praying for my daughter’s miracle healing, I wasn’t prepared for ALL the ways that God would answer that prayer…silly me! From the moment we knew there was a problem in the womb, we began praying that God would instantly and miraculously heal our baby girl; and for…
Learn more about Hope's case -

Harper Neenah, Wisconsin, United States Fibular Hemimelia
Harper was born with a rare orthopedic condition, fibular hemimelia. Her left leg is shorter than her right, with most of the discrepancy in her tibia, but also some in the femur. Her predicted discrepancy at maturity is 15 cm. In addition to limb length discrepancy, she was born with foot and ankle deformity. As…
Learn more about Harper's case -

Haley Nebraska, United States Congenital Femoral Deficiency
I can only say good things about our experience with the Paley Institute. When Haley was six weeks old, the Shriners wanted to amputate her leg. She was born with proximal focal femoral deficiency (PFFD), also known as congenital femoral deficiency (CFD). I found Dr. Paley and he looked at her and said with no…
Learn more about Haley's case -

Gillian Washington, D.C., DC, United States Achondroplasia
Looking Back on 25 Years from Uhuru PeakSeptember 28, 2013The sun was bright, the sky was blue and the air was cold as I looked down from Uhuru peak, the highest point in Africa. The summit was crowded and I was tired so it was hard to reflect on the meaning of it all, but…
Learn more about Gillian's case -

Evan Victoria, Minnesota, United States Congenital Femoral Deficiency
We started our relationship with the Paley Institute when Evan was less than 1 year old. It started with an exploratory email to Dr. Paley while he was lecturing in Europe. He responded to our email within 45 minutes and said he would review Evan’s x-rays and an MRI as soon as he returned home.…
Learn more about Evan's case -
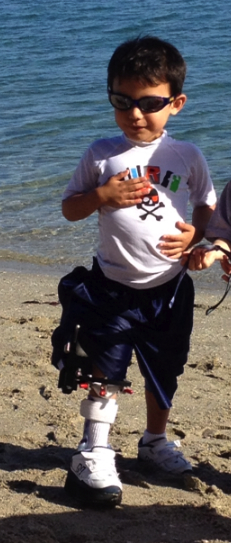
Ethan Red Oak, Texas, United States Congenital Femoral Deficiency
When our son Ethan was born, we were filled with joy. We had a tough pregnancy and just seeing his face healthy and strong filled us with excitement. Prior to being discharged, his pediatrician diagnosis was Proximal Femoral Focal Deficiency (short right femur) and advised us to go see an orthopedic surgeon at Scottish Rite…
Learn more about Ethan's case -
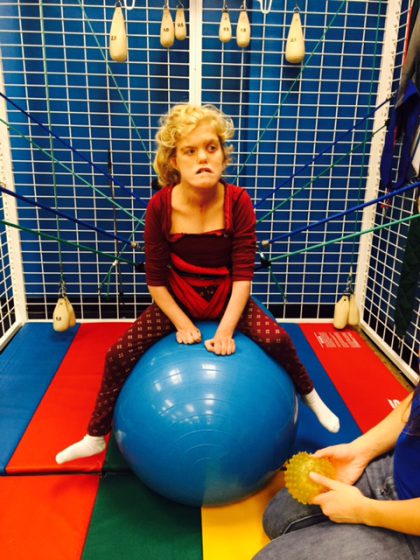
Erika Northport, New York, United States CHARGE Syndrome
Erika was born June 30, 1995 with CHARGE Syndrome, a medically rare and very complex syndrome. At the age of 20 she has endured over 52 surgeries. At the age of one, she had her second heart surgery; post operatively, she went into blood pressure arrest followed by cardiac arrest. The “stroke” caused brain damage…
Learn more about Erika's case -
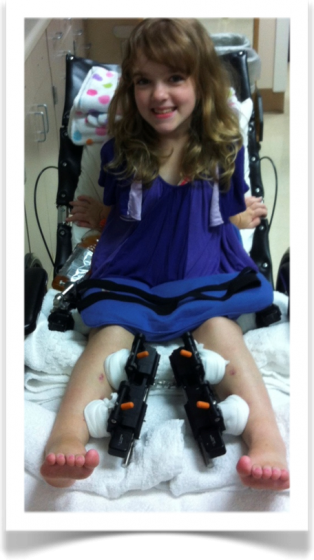
Emma Fargo, North Dakota, United States Achondroplasia
Emma's Letter Dear Dr. Paley, No words can explain how thankful I am for everything you have done for me. The 16 inches you have given me in my legs and the 4 inches you have given me in my arms will help me live the rest of my life independently. Without you, I would…
Learn more about Emma's case -

Emma West, Mississippi, United States Osteomyelitis
Emma has been a patient of Dr. Robbins since she was five. We were referred to him by Dr. Purvis after she suffered osteomyelitis in her tibia arresting her growth plate at 4 years of age. Dr. Robbins led us down this crazy road of lengthening and introduced us to the fixator. He has done…
Learn more about Emma's case -

Emily New York, NY, United States Hip Dysplasia
Dr. Feldman literally saved my life. He saved my ability to do everything I need and want to without having to worry about the future.I loved to run, but I started to have pain in my groin and hip when I ran long distances. I couldn’t lift my leg to get in to my car.…
Learn more about Emily's case -

Emily Middletown, Connecticut, United States Congenital Femoral Deficiency
The first six months of our daughter’s life were anything but typical. When she was two hours old, our doctor sat down in front of us with a pile of papers and a concerned look, telling us x-rays had shown Emily’s right femur to be significantly shorter than her left, most likely the result of…
Learn more about Emily's case -

Dylan Midlothian, Virginia, United States Multiple Hereditary Exostoses
Our son Dylan, who is now 15, was first diagnosed with MHE at age 5. We noticed a large bump on his knee that was not going away but getting bigger in size. Since that time we have seen 4 different pediatric orthopedic surgeons in the greater Richmond area who provided the same response….not much…
Learn more about Dylan's case -

Douglas New York, NY, United States Arthrogryposis
I was sitting in my Mom’s belly pretzel style before I was born. My legs and feet were tangled up together. My legs, feet, arms and hands had tight joints. The problem is called Arthrogryposis. My Mom and Dad were very worried when I was born. They did not know if I would stand, walk,…
Learn more about Douglas's case -

Demi Palm Beach Queensland, Australia Fibular Hemimelia
We discovered our daughter Demi had a problem with her right leg 18 weeks into the pregnancy during a routine scan. After multiple ongoing scans doctors were unable to provide a definitive diagnosis, we were told it could be anything from a single missing bone to brittle bone disease. When our daughter was born…
Learn more about Demi's case -

David Minnesota, United States Avascular Necrosis of the Hip
On July 14, 2013 I was on the last day of an eight day canoeing/portage trek called the Northern Tier in the boundary waters in Minnesota as part of the Boy Scouts of America high adventure program. This was the last leg in what was to earn me the Triple Crown of high adventure in…
Learn more about David's case -

Caroline New York, NY, United States Arthrogryposis
Our daughter Caroline is a miracle. She has defied every odd since the day of her birth. She is courageous, resilient, strong, tough, determined. Brave. If she were a story book, she would be “The Little Engine That Could.” If she were a word it would be Hope. She was born premature and still, unable…
Learn more about Caroline's case -

Brian Sausalito, California, United States Growth Arrest
Even though the discrepancy in my leg lengths was just over a half inch, I chose to lengthen my short leg to achieve symmetry. In my case, the cost was well worth the effort. The short leg was creating scoliosis in my spine, which led to a number of physical problems, slowing me down and…
Learn more about Brian's case -

Bernard New Jersey, United States Perthes Disease
In March, 2011 my 8 year old son was diagnosed with Perthes Disease and referred to a specialist to plan his treatment. At the time, I had no idea what that meant. After 2 conflicting opinions about the course of treatment for my son, I reached out to his pediatrician for guidance. She urged me…
Learn more about Bernard's case -

Baylee Strasburg, Virginia, United States CHARGE Syndrome
Baylee was born Oct 23 2012 with CHARGE Syndrome. Charge Syndrome is very rare. It is caused by a genetic anomaly.Baylee has Coloboma of both eyes, She has had surgery for mal rotation of her intestines and an appendectomy at one day old, she is profoundly deaf in both ears, she has an absent right…
Learn more about Baylee's case -

Axel New Jersey, United States Arthrogryposis
We were completely devastated when we took our son Axel, 4 days old to Doctor David Feldman. When he was born, the Pediatrician told us straight that she had never seen a case like this before. What we only knew was that he had severe bilateral clubfeet and what we could all see was that…
Learn more about Axel's case -

Ashley New York, NY, United States Scoliosis
Ashley is 13 years old. This past summer she hiked 7.5 miles 5,000 feet up in elevation out of the Grand Canyon, and 8.2 miles 4,000 feet down in elevation from Glacier Point in Yosemite National Park. Besides her love of hiking, Ashley is a Competitive Swimmer, Soccer Player and Ballet Dancer. For the past…
Learn more about Ashley's case -

Apollonia Ottawa, ON, Canada Tibial Hemimelia
Today, Dr. Paley is Apollonia`s surgeon and our family’s hero. The day we met Dr. Paley I knew Apollonia would keep her leg. This story is likely just one of many that you will hear, but for our Italian-Canadian family living in Ottawa, Canada, it is a cherished one.When our daughter Apollonia was born with…
Learn more about Apollonia's case -

Anthony New Jersey, United States Perthes Disease
My name is AJ and I am a patient of Dr Feldman for many years. Right before my fourth birthday in 2003, I was diagnosed with bilateral Perthes Diseases. I can remember the agonizing pain when I tried to walk or simply stand. One morning I couldn’t get out of bed. I was unable to…
Learn more about Anthony's case -

Anna Poznań, Poland Congenital Pseudarthrosis of the Tibia
I am Anna, a Polish 3 year-old girl. I was born in 2009 with a genetic disease NF 1 which affected CPT of the left leg. My parents were shocked when they had been told that in first year of my life the leg would be broken and never united by itself. That happened very…
Learn more about Anna's case -
Angelica Milan, Italy Avascular Necrosis of the Hip
Angelica (we call her Jay) fell out of a window in our country house on the outskirts of Milan, Italy from a height of nine meters on the 3rd of March, 2007. She had just turned three. Jay survived, but had multiple fractures at her pelvis and the neck of the femur. “It’s only bones,”…
Learn more about Angelica's case -

Alisa Moscow, Russia Congenital Femoral Deficiency
When our daughter Alisa was born in 2006 with congenital short hip deformity, we were in shock. We spent about two months looking for a doctor in Moscow, where we live, who could explain Alisa’s diagnosis and prospects. Although Russia is the country where Ilizarov’s method was invented, doctors would simply shrug their shoulders, suggesting…
Learn more about Alisa's case -

Aiden Florida, United States Congenital Femoral Deficiency
Aiden was born on May 12, 2010, He was born with Congenital Femur Deficiency; which such diagnostics we did not know of until we met Doctor Dror Paley. Everywhere we went the answer was “amputation”. This absurd conclusion was not what we wanted to hear; therefore we continued our desperate search. Our search went on…
Learn more about Aiden's case -

Andrea Venezuela Fibular Hemimelia
I want to share a human story. In this convulsed world of ours things happen that teach us that love and happiness have not disappeared and that we must never lose faith that wonderful and generous people will always be around.Andrea, my first granddaughter, was born on September 24th 1998. Four months before she was…
Learn more about Andrea's case -

Adina Romania Multiple Hereditary Exostoses
My name is Adina and I have MHE. I’m from Romania, but I live in California. My mom discovered a bump on my left hand when I was 5. It took her more than 1 year to find a doctor who diagnosed me. Since then I had 10 surgeries on my knees and arms (9…
Learn more about Adina's case -

Abigail Madison, Alabama, United States Fibular Hemimelia
I clearly remember the first day we found out that our perfect little girl had an issue with her leg. We were at one of our first few ultrasounds, where they were counting bones, fingers, toes, etc. Abigail, being our first child, we were not very sure exactly what we were looking at, but one…
Learn more about Abigail's case -

Abdul Riyadh, Riyadh Province, Saudi Arabia Congenital Femoral Deficiency, Fibular Hemimelia
(translated from Arabic) My name is Abdulhakim Almadi, a 37 year-old male from Saudi Arabia. I was born with a combination of a congenital short femur and short tibia with absent fibula. In 1982, I underwent a surgery in London, UK to stabilize my right hip joint, which was the immediate problem then. Later on,…
Learn more about Abdul's case -
Patient(s) treated from:
Chapais, QC, Canada
-
Patient(s) treated from:
Labrador City, NL, Canada
-
Patient(s) treated from:
Kingaroy, Queensland, Australia
-
Patient(s) treated from:
Sunshine Coast, Queensland, Australia
-
Patient(s) treated from:
Brisbane, Queensland, Australia
-
Patient(s) treated from:
Alice Springs, Northern Territory, Australia
-
Patient(s) treated from:
Perth, Western Australia, Australia
-
Patient(s) treated from:
Canberra, Australian Capital Territory, Australia
-
Patient(s) treated from:
New Caledonia
-
Patient(s) treated from:
Papua New Guinea
-
Patient(s) treated from:
Timor-Leste
-
Patient(s) treated from:
Arkhangelsk, Arkhangelsk Oblast, Russia
-
Patient(s) treated from:
Greece
-
Patient(s) treated from:
St Petersburg, Saint Petersburg, Russia
-
Patient(s) treated from:
Latvia
-
Patient(s) treated from:
Herning, Denmark
-
Patient(s) treated from:
Karlstad, Sweden
-
Patient(s) treated from:
Copenhagen, Denmark
-
Patient(s) treated from:
Stockholm, Sweden
-
Patient(s) treated from:
Bergen, Norway
-
Patient(s) treated from:
Reykjahlíð, Iceland
-
Patient(s) treated from:
Reykjavík, Iceland
-
Patient(s) treated from:
Olenyok, Sakha Republic, Russia
-
Patient(s) treated from:
Ekonda, Krasnoyarsk Krai, Russia
-
Patient(s) treated from:
Serov, Sverdlovsk Oblast, Russia
-
Patient(s) treated from:
Nizhny Novgorod, Nizhny Novgorod Oblast, Russia
-
Patient(s) treated from:
Jessore, Khulna Division, Bangladesh
-
Patient(s) treated from:
Dhaka, Dhaka Division, Bangladesh
-
Patient(s) treated from:
Yangon, Yangon Region, Myanmar (Burma)
-
Patient(s) treated from:
Cagayan de Oro, Northern Mindanao, Philippines
-
Patient(s) treated from:
Hong Kong
-
Patient(s) treated from:
Hanoi, Vietnam
-
Patient(s) treated from:
Nha Trang, Khanh Hoa Province, Vietnam
-
Patient(s) treated from:
Phnom Penh, Cambodia
-
Patient(s) treated from:
Brunei
-
Patient(s) treated from:
Kuala Lumpur Federal Territory of Kuala Lumpur Malaysia
-
Patient(s) treated from:
Taiwan
-
Patient(s) treated from:
Yuxi, Yunnan, China
-
Patient(s) treated from:
Guiyang, Guizhou, China
-
Patient(s) treated from:
Tokyo, Japan
-
Patient(s) treated from:
Wuhan, Hubei, China
-
Patient(s) treated from:
Beijing, China
-
Patient(s) treated from:
Seoul, South Korea
-
Patient(s) treated from:
Daegu, South Korea
-
Patient(s) treated from:
North Korea
-
Patient(s) treated from:
Songino Khairkhan, Ulaanbaatar, Mongolia
-
Patient(s) treated from:
Ulan Bator, Ulaanbaatar, Mongolia
-
Patient(s) treated from:
Tajikistan
-
Patient(s) treated from:
Cyprus
-
Patient(s) treated from:
Bhutan Post, Thimphu, Bhutan
-
Patient(s) treated from:
Baghdad, Baghdad Governorate, Iraq
-
Patient(s) treated from:
Tehran, Tehran Province, Iran
-
Patient(s) treated from:
Damascus, Damascus Governorate, Syria
-
Patient(s) treated from:
Jerusalem, Israel
-
Patient(s) treated from:
Amman, Amman Governorate, Jordan
-
Patient(s) treated from:
Bahrain
-
Patient(s) treated from:
Qatar
-
Patient(s) treated from:
Mecca, Makkah Province, Saudi Arabia
-
Patient(s) treated from:
Bishah, Aseer Province, Saudi Arabia
-
Patient(s) treated from:
Ahmedabad, Gujarat, India
-
Patient(s) treated from:
Kathmandu, Central Development Region, Nepal
-
Patient(s) treated from:
New Delhi, Delhi, India
-
Patient(s) treated from:
Pakistan
-
Patient(s) treated from:
Afghanistan
-
Patient(s) treated from:
Ashgabat, Turkmenistan
-
Patient(s) treated from:
Tashkent, Uzbekistan
-
Patient(s) treated from:
Kyrgyzstan
-
Patient(s) treated from:
Kazakhstan, Astana
-
Patient(s) treated from:
Kharkiv, Kharkiv Oblast, Ukraine
-
Patient(s) treated from:
Austria
-
Patient(s) treated from:
Berlin, Germany
-
Patient(s) treated from:
Hanover, Germany
-
Patient(s) treated from:
Wales, England, United Kingdom
-
Patient(s) treated from:
United Kingdom, England, London
-
Patient(s) treated from:
Manchester, United Kingdom
-
Patient(s) treated from:
Newcastle upon Tyne, England, United Kingdom
-
Patient(s) treated from:
Scotland
-
Patient(s) treated from:
France
-
Patient(s) treated from:
Bulgaria
-
Patient(s) treated from:
Serbia
-
Patient(s) treated from:
Yemen
-
Patient(s) treated from:
Sudan
-
Patient(s) treated from:
Egypt, Cairo
-
Patient(s) treated from:
Libya, Tripoli
-
Patient(s) treated from:
Tunisia
-
Patient(s) treated from:
Algiers
-
Patient(s) treated from:
Portugal, Lisbon
-
Patient(s) treated from:
Spain, Madrid
-
Patient(s) treated from:
Morocco, Casablanca
-
Patient(s) treated from:
Guelmim, Guelmim-Es Semara, Morocco
-
Patient(s) treated from:
Gambia
-
Patient(s) treated from:
Guinea-Bissau
-
Patient(s) treated from:
Praia, Cape Verde
-
Patient(s) treated from:
Sierra Leone, Freetown
-
Patient(s) treated from:
Burkina Faso
-
Patient(s) treated from:
Nigeria
-
Patient(s) treated from:
Togo
-
Patient(s) treated from:
Cameroon
-
Patient(s) treated from:
Darki, Chad
-
Patient(s) treated from:
Djibouti
-
Patient(s) treated from:
Addis Ababa, Ethiopia
-
Patient(s) treated from:
Mogadishu, Somalia
-
Patient(s) treated from:
Burundi
-
Patient(s) treated from:
Lusaka, Lusaka Province, Zambia
-
Patient(s) treated from:
Botswana
-
Patient(s) treated from:
Zimbabwe
-
Patient(s) treated from:
Victoria, Mont Fleuri, Seychelles
-
Patient(s) treated from:
Port Louis, Mauritius
-
Patient(s) treated from:
Madagascar
-
Patient(s) treated from:
Maseru, Lesotho
-
Patient(s) treated from:
Cape Town, Western Cape, South Africa
-
Patient(s) treated from:
Trinidad and Tobago
-
Patient(s) treated from:
Kingstown, Saint George, Saint Vincent and the Grenadines
-
Patient(s) treated from:
Roseau, Saint George Parish, Dominica
-
Patient(s) treated from:
Antigua and Barbuda
-
Patient(s) treated from:
Saint Kitts and Nevis
-
Patient(s) treated from:
San Juan, Puerto Rico
-
Patient(s) treated from:
Santo Domingo, Santo Domingo Province, Dominican Republic
-
Patient(s) treated from:
Haiti, Port-au-Prince
-
Patient(s) treated from:
Concepción, Chile
-
Patient(s) treated from:
Santiago, Chile
-
Patient(s) treated from:
Neuquen, Argentina
-
Patient(s) treated from:
Buenos Aires, Argentina
-
Patient(s) treated from:
Asuncion, Paraguay
-
Patient(s) treated from:
Concepcion, Paraguay
-
Patient(s) treated from:
Brasília - Federal District, Brazil
-
Patient(s) treated from:
Alta Floresta - State of Mato Grosso, Brazil
-
Patient(s) treated from:
Lima District, Lima Region, Peru
-
Patient(s) treated from:
Cali - Valle del Cauca, Colombia
-
Patient(s) treated from:
Ecuador
-
Patient(s) treated from:
Panama City, Panama
-
Patient(s) treated from:
Culiacán, Mexico
-
Patient(s) treated from:
Rock Springs, Wyoming, USA
-
Patient(s) treated from:
Portland, Oregon, USA
-
Patient(s) treated from:
Vancouver, BC, Canada
-
Patient(s) treated from:
Victoria, BC, Canada
-
Patient(s) treated from:
Winnipeg, Manitoba, Canada
-
Patient(s) treated from:
Prophet River, BC, Canada
-
Patient(s) treated from:
Gustavus, Alaska, USA
-
Patient(s) treated from:
Takotna, Alaska, USA
Centers of Excellence
Each doctor at the Paley Orthopedic & Spine Institute specializes in a specific area of orthopedics.
Below are our centers of excellence.
The Team of Paley Specialists Let us introduce you to our team!
The Paley Orthopedic & Spine Institute offers coordinated, concierge care throughout all stages of treatment. Our entire staff of over 40 employees, including physicians, physician assistants, medical assistants, physical and occupational therapists, orthopedic technologists, and office staff, all work in one building: the Kimmel Building, on the campus of St. Mary’s Medical Center. This allows our staff to communicate quickly and effectively, ensuring the highest level of coordinated care for each of our patients.

The unLIMBited Foundation
The unLIMBited Foundation is committed to helping children and adults with rare and complicated orthopedic problems.
We advocate for limb saving and life changing, proven medical treatments that emphasize reconstruction over amputation.

